How to Treat Skin Conditions; Eczema, Seborrhea and Psoriasis
Physical Health
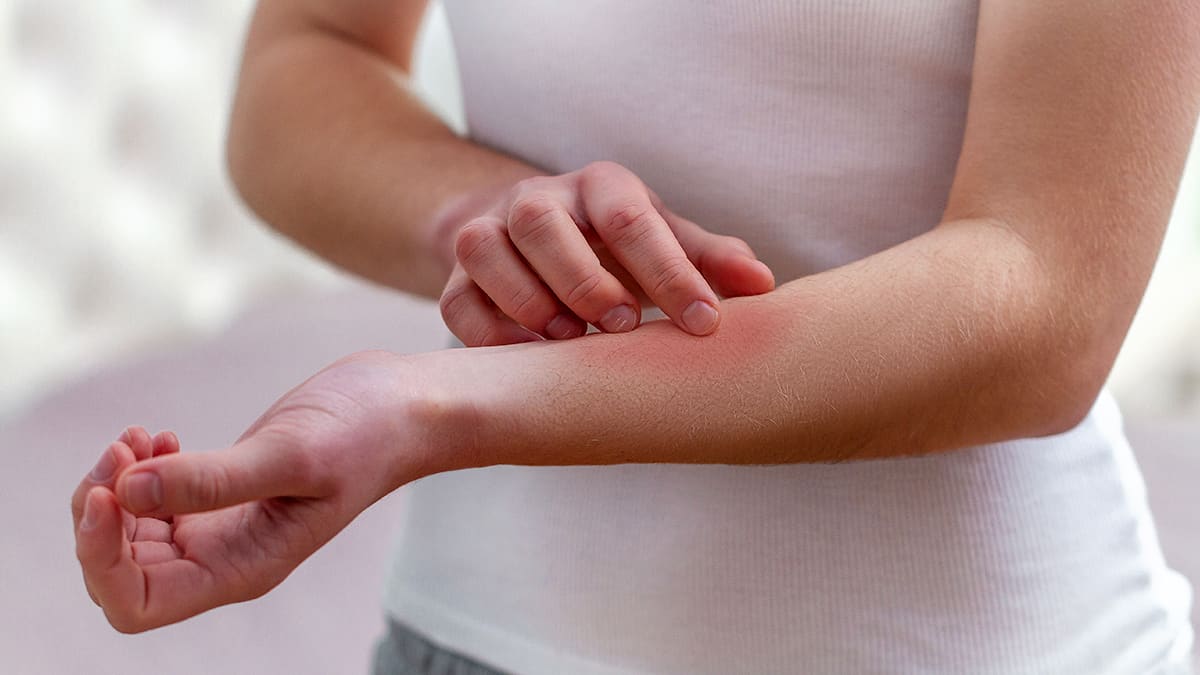
Eczema, seborrhea, and psoriasis are health conditions that lead to irritated skin and scaly, itchy rashes. These conditions are all autoimmune diseases, involving the immune system. While normally the immune system’s job is to fight off infection, in these conditions, something causes the immune system to go into overdrive and begin attacking the body’s own cells. Eczema, seborrhea, and psoriasis are thought to have slightly different causes, but they are often managed using some of the same types of treatments.
What Is Eczema?
Close to 1 in 3 people have eczema at some point in their life. This condition is not contagious, meaning that you can’t spread eczema to other people.
What Does Eczema Look Like?
There are a few different types of eczema. The most common is atopic dermatitis, which causes certain areas of your skin to become very itchy. You may have patches of skin that look:
- Swollen
- Cracked
- Scaly
- Crusted
- Red
People generally have eczema for a very long time. It is not usually a rash that appears suddenly and goes away quickly. Many people with eczema have had this condition since they were children.
What Causes Eczema?
Doctors don’t know for sure what causes this condition. They think eczema may be partly caused by genes that you inherit from your parents, meaning that eczema may run in families. This disorder is also probably partially caused by things in your environment that irritate your skin.
What is Seborrhea?

About 5% of people around the world have seborrhea, also called seborrheic dermatitis. However, one particular form of seborrhea, dandruff, is far more common. Dandruff doesn’t involve as much inflammation as does traditional seborrhea, and it only occurs on the scalp. Up to half of the world’s population has experienced dandruff.
What Does Seborrhea Look Like?
Seborrhea usually appears on the face or scalp, as well as on the trunk and in between body folds. Adults with seborrhea often have raised patches that appear reddish in pale-skinned people and as darker areas in darker-skinned people. These patches are often covered with yellowish, crusted scales. They may also be oily or greasy, and may itch.
Seborrhea also occurs in infants, where it may cause a non-itchy, non-painful rash on the face, head, trunk, and diaper area. Many infants with seborrhea have a condition called cradle cap, in which patches covered with yellowish scales appear on the head. Cradle cap usually develops when the infant is 3 months old or less, and goes away on its own after a few months.
Dandruff usually results in white or yellow flakes coming off of the scalp. Some people with dandruff also have redness or itching on the skin of the head, underneath the eyebrows, or behind the ears.
What Causes Seborrhea?
Experts still don’t fully understand the causes of seborrhea. However, they have identified some of the factors that may be involved. These include:
- Yeast: this is a type of fungus that normally lives on the skin. Researchers have found that people with dandruff or seborrhea often have higher numbers of certain types of yeast on their skin.
- Sebaceous glands: these are small structures within the skin that make an oily substance. This substance helps protect the skin and hair and keep it healthy. People with seborrhea may have sebaceous glands that are too active and produce too much oil.
- Genetics: the genes that are passed down from your parents may affect how likely you are to get seborrhea. Genes control things like how thick your skin is and how your immune system works. These factors in turn can affect whether you get seborrhea.
What Is Psoriasis?
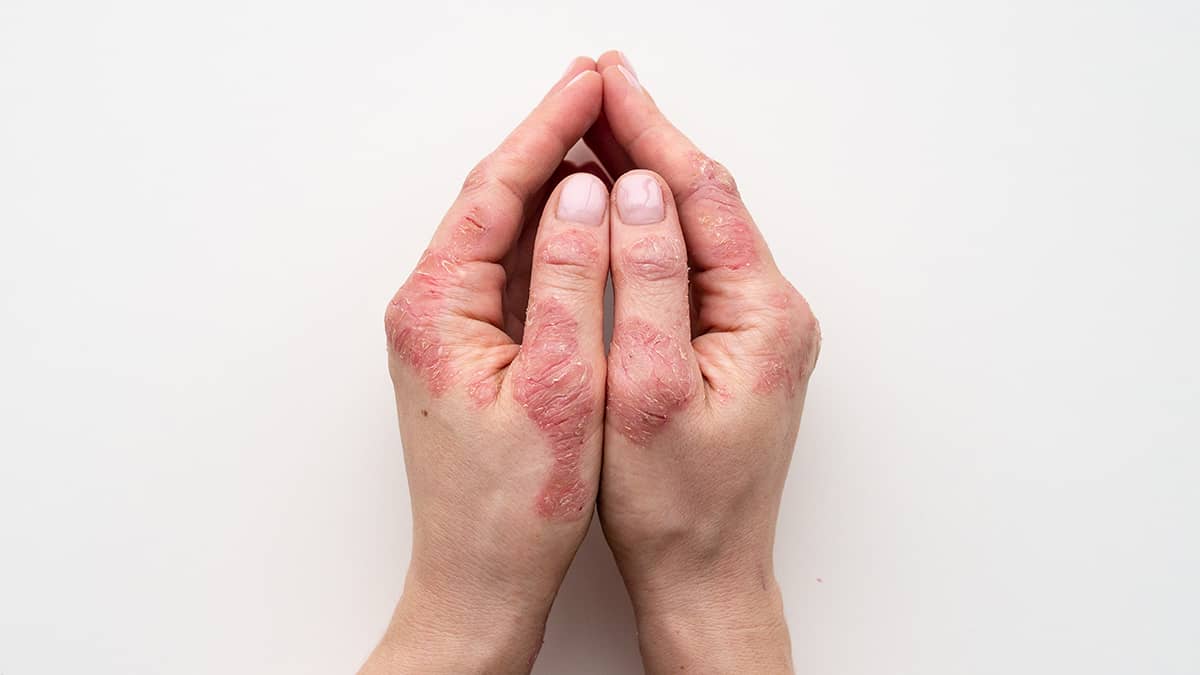
Researchers estimate that about 2-3% of people around the world have psoriasis. About 10-20% of people with this condition also develop psoriatic arthritis, a related disorder that causes joint pain
What Does Psoriasis Look Like?
Psoriasis leads to patches on the skin. These most often appear on the knees, elbows, hands, feet, back, face, or scalp. These patches are usually darker in color than your normal skin, appearing pinkish, reddish, or darker brown. They may also be covered with silver or gray flakes or scales. Your skin is often thicker in these patches, and may feel itchy. People with psoriasis also frequently have dandruff and small holes or dents in the fingernails or toenails.
What Causes Psoriasis?
As is the case for eczema and seborrhea, experts still aren’t exactly sure what causes psoriasis. In this condition, inflammation seems to cause new skin cells to grow too quickly. Psoriasis runs in families, indicating that genetics may play a role. Additionally, other factors can also make someone more likely to get psoriasis:
- A physical injury of the skin, such as a cut, burn, bug bite, or tattoo
- Certain medications, including beta blockers, non-steroidal anti-inflammatory drugs such as aspirin and ibuprofen, and drugs that change the immune system
- Infections, including strep throat
- High levels of certain types of bacteria or yeast on the skin
- Drinking high amounts of alcohol or smoking
Keeping Eczema, Seborrhea, and Psoriasis Flares Under Control

Inflammatory skin conditions typically have symptoms that come and go. Sometimes, these diseases become more active, causing symptoms to worsen. These periods are called “flares.” Other times, symptoms will go into remission – they will lessen or even disappear. One key aspect of treating eczema, seborrhea, and psoriasis is to stop flares from coming on.
Managing Dry Skin
Studies have found that people living in colder climates often have more flares from eczema, seborrhea, and psoriasis during the colder months, when the air is drier. Therefore, one of the goals of treating these conditions is to keep dry skin under control. You can practice good skin care by:
- Applying a moisturizing lotion a few times per day, especially after bathing, in order to keep your skin from drying out. Try using a lotion that doesn’t contain any dyes, fragrances, or other chemicals.
- Using a humidifier, especially during the colder months, to keep the air from getting too dry.
- Trying not to scratch your skin. Keep your nails short or wear gloves to avoid the temptation to scratch. Instead, apply an anti-itch cream.
On the other hand, getting too much sun can also worsen symptoms of these conditions. Make sure to protect your skin by applying sunscreen when you go outside.
Preventing Skin Irritation
Many times, conditions like eczema get worse when your skin comes into contact with certain materials that make it irritated. Some people have reactions to specific kinds of soap, laundry detergent, fabric, or skin products. However, it may be hard to identify which of these things is causing flares. Consider things like:
- Did you recently start using a new lotion or a new facial product?
- Did someone in your household recently start using a different brand of laundry detergent, fabric softener, or dryer sheets?
- Have you been regularly using a different new kind of hand soap, at home or at work?
Seborrhea and psoriasis may also worsen when the skin becomes irritated. Certain skin medications, such as fluorouracil, and certain cosmetic products may lead to seborrhea flares. Additionally, psoriasis flares have been linked to skin injuries like cuts and burns.
Do your best to protect your skin from potential damage. Try wearing gloves when doing tasks around the house like cleaning or gardening. If you have frequent flares, try switching out skin care, cleaning, and soap products one at a time and replacing them with another brand or a different type of product. This may help you see if any of these products are contributing to your symptoms.
Managing Stress
Eczema, seborrhea, and psoriasis flares have all been linked to stress. When the body is stressed, it makes certain hormones – natural substances in the body that act as messengers. These hormones may affect both the immune system and skin cells, leading to inflammation and skin symptoms.
Working to reduce stress and better manage your mental health may help your skin symptoms improve. Here are some ideas for getting your stress levels under control:
- If you have a lot you need to get done at home, work, or school, try making a to-do list in order to keep track of your responsibilities. Be realistic about how much you can get done.
- Develop healthy habits, such as eating healthy foods (especially superfoods), exercising, and getting more sleep, in order to lower stress levels.
- Learn how to relax. Try stretching, deep breathing, or meditation exercises in order to calm your body and your mind.
- Avoid alcohol and drugs. This can sometimes cause more negative feelings in the short term, but helps improve your mental health in the long run.
- Tell your loved ones when you’re feeling overwhelmed. Talking with a friend or family member can help you better deal with stress.
- If your stress levels or mental health seem to be getting worse, you may get best results by talking to a professional. Try talking to a doctor, counselor, social worker, or therapist.
Treatments for Eczema, Seborrhea, and Psoriasis
The treatment you receive for a skin condition may depend on different factors, such as which areas of your skin are affected and how severe your symptoms are. You may have to try a few different strategies before you find a treatment plan that works for your skin.
Topical Medications
Eczema, seborrhea, and psoriasis are often treated with topical medications. “Topical” refers to something that is applied directly to the skin. Many topical skin creams containing different medications have been developed to help treat inflammation.
When diagnosed with eczema, seborrhea, or psoriasis, many people are first prescribed a corticosteroid treatment. Steroids calm the immune system and stop skin cells from growing and dividing so quickly. They may come in the form of ointments, creams, gels, foams, or lotions. Steroids keep skin conditions under control for many people, but don’t work for everyone. Additionally, steroids should only be taken temporarily, and are not a long-term solution.
If you need to try a different treatment, your doctor may give you other topical medications:
- Topical immunomodulators (TIMs) are medications that change the way in which the immune system interacts with the skin. Examples of TIMs used to treat inflammatory skin problems include tacrolimus and pimecrolimus.
- Skin cream containing coal tar is frequently used to treat eczema and psoriasis. It may help eliminate inflammation and make skin cells grow more slowly.
- Topical treatments that contain ceramides may help. Ceramides are a type of fat molecule that allow the skin to work properly. People with inflammatory skin conditions may have ceramides that don’t function correctly, so applying ceramides as a treatment may help treat these conditions.
- Treatments with lactic acid or salicylic acid can help reduce skin scales.
- Antibiotics can fight off germs if you have developed an infection within your skin.
- Anti-fungal treatments such as ketoconazole can help keep the yeast that grows on your skin under control.
Medications Taken by Mouth
For more severe cases of eczema, seborrhea, and psoriasis, skin treatments may not be enough to reduce symptoms. Oral medications (pills taken by mouth) may be prescribed. Examples of possible oral treatments include antihistamines (allergy medication), steroid medications, anti-fungal treatments, vitamin A or vitamin D treatments, and drugs that slow down the immune system.
Biologics
A newer category of treatments called biologics has recently been developed to help with inflammatory skin problems. Biologics can block specific immune cells or molecules that cause inflammation. These drugs may be taken as a skin cream, oral medication, or other methods. For example, for more severe cases of eczema, a drug called dupilumab can be injected under the skin. A wide variety of biologics have also been approved to treat psoriasis. These include adalimumab (Humira) and ustekinumab (Stelara). Researchers are also beginning to study how biologics may help people with seborrhea. If you are interested in seeing how biologics may work for you, talk to your doctor.
Light therapy
Many doctors recommend light therapy, also called phototherapy, to help with eczema, seborrhea, and psoriasis. During this treatment, you are exposed to ultraviolet (UV) light either over your whole body or just in one specific affected area. UV light can lessen inflammation, make skin cells grow more slowly, and soothe symptoms of eczema, seborrhea, and psoriasis.
Certain forms of UV light can make the skin age faster and can lead to a higher chance of getting cancer. Your doctor can determine the right types and dose of UV light to provide while maximizing benefits and minimizing risks. For this reason, it is important to receive these treatments in a hospital or doctor’s office. Light therapy isn’t the same as using a tanning bed, which are more likely to damage your skin.
Shampoos for Dandruff
When you have seborrhea on the scalp (dandruff), special shampoos can usually solve the problem. Studies have found that shampoos containing medication like ketoconazole, ciclopirox, selenium sulfide, coal tar, zinc pyrithione, salicylic acid, and tacrolimus can help reduce symptoms. Some of these options are available over-the-counter at your local store, while others need a prescription from a doctor.
Conclusion
Conditions like eczema, seborrhea, and psoriasis are often hard to tell apart from each other. If you think you have one of these conditions, it may help to see a doctor so that you can be sure you are using the right treatments. Your doctor can more accurately tell which condition you have by looking at your skin and asking you about other possible symptoms. Your doctor may also use a biopsy to diagnose you. In order to take a biopsy, your doctor will take a small sample of your skin and then look more closely at your skin cells under a microscope in order to get a better idea of what’s going on.
Your doctor can also help you come up with a treatment plan. Many people with eczema, seborrhea, and psoriasis need to use a variety of strategies in order to come up with something that helps. Reducing how often flares pop up and treating symptoms when they appear can help you better manage your skin condition.