Doctors diagnose one in four U.S. women during their lives with a pelvic floor disorder. If you’re not sure what or where the pelvic floor is, it’s a remarkable set of muscles and tissue that form a sling or “hammock” around the pelvic floor. It protects the pelvic organs, including the bladder, small bowel, and rectum. It also supports the uterus and vagina in women and the prostate in men. The pelvic floor helps with important functions such as urinating and defecating, sexual intercourse, and childbirth. Keep reading to learn more about the muscles and tissues of the pelvic floor. Then find out which problems can develop when they’re too tight or weak, and discover how to prevent or treat them.
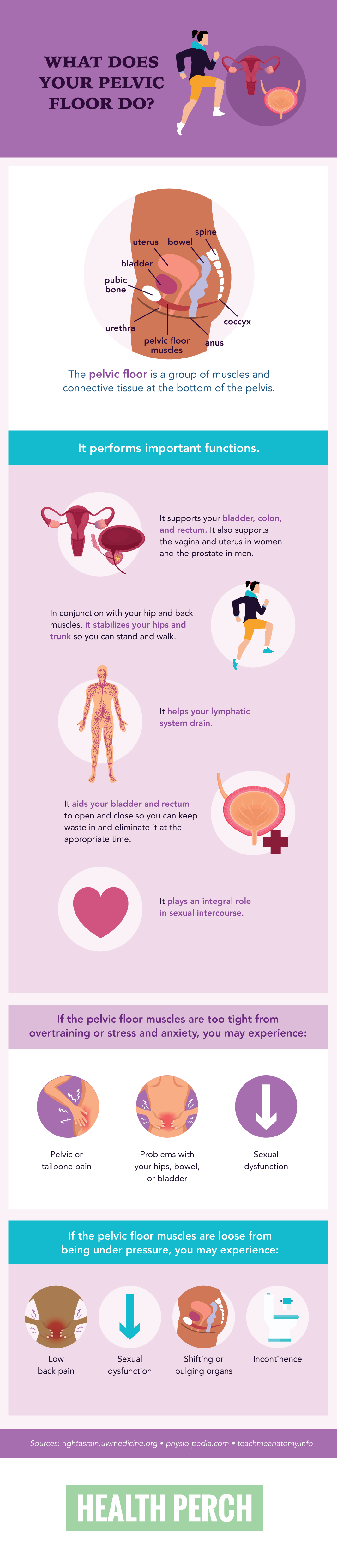
Pelvic Floor Dysfunctions
The pelvic floor can be prone to pelvic floor dysfunction (PFD). Like any muscles, the pelvic floor muscles can weaken over time from a variety of circumstances. Weak muscles can contribute to pain and incontinence. In addition to relaxing or weakening, these muscles can also become tight and constricted, which can make it difficult to evacuate the bowels properly or completely and lead to leaking of urine or stool.
Several factors can cause PFD.
The extra weight of a baby puts pressure on the pelvic floor, and strain and pushing during labor aggravates these muscles and tissues.
Overly tight pelvic floor muscles can cause constipation, which is the inability to regularly or completely empty the bowels. And chronic constipation can lead to weakened pelvic floor muscles from repeated straining and pushing of the muscles that help evacuate the bowel.
People who lift heavy weights for a job or do intense weightlifting exercises may strain their pelvic floor muscles. Learn to lift with your legs, and be careful if you feel straining during lifting.
Intense exercise that involves jumping or gymnastic movements, especially when both feet come off the ground, can put extra pressure on the pelvic floor. Work with a physical trainer to modify exercises.
Researchers have linked excess weight, particularly obesity, to increased pressure on the pelvic floor. Health care providers may recommend weight loss as the first line of treatment to address any PFD.
- Smoking
Smoking may contribute to pelvic floor disorders in two ways. It can cause chronic coughing that strains pelvic muscles. And it can irritate the bladder and even increase the risk of bladder cancer.
When women’s menstrual cycles cease at menopause, estrogen and progesterone hormones diminish, which may reduce the strength and elasticity of muscles and tissues in the pelvic floor, leading to disorders. However, researchers have not definitively established that menopause causes PFDs.
The common symptoms of pelvic floor disorders vary and may seem minor, but you may mention any of the following to your healthcare professional.
- Heaviness, fullness, or pulling in the pelvic region.
- Leaking urine or stool
- Pain during urination or sex
- Difficulty emptying the bladder completely
- Constipation
- Frequent urinary tract infections
Pelvic Floor Solutions
Pelvic floor issues are common, but they’re not necessarily normal or inevitable. Talk to your health care provider about these preventative measures and treatments.
As the first step toward a healthier pelvic floor, it may help to make some changes to your diet and lifestyle. For instance, you may want to avoid caffeinated or carbonated beverages that stimulate the bladder. Adding fiber to your diet prevents constipation. Losing weight takes pressure off your bladder and pelvic organs. And if you smoke, quitting can reduce chronic coughing and take pressure off your pelvic floor.
You may need to train your pelvic floor muscles as you do other muscles. As mentioned, some symptoms may be signs your pelvic floor is too tense. Biofeedback or breathing techniques can help you learn to relax tight muscles. Bladder training, which involves urinating at specific times of day, can help you regain bladder control. And if your pelvic floor muscles are weak, kegel exercises can help you strengthen them.
A pelvic floor physical therapist can work with you to learn how to strengthen or loosen your muscles. Pelvic floor physical therapy (PFPT) may involve manual therapy, biofeedback, electrical stimulation, behavioral education, and home exercise programs.
Your doctor may also recommend medication if you’re having a hard time with bladder or bowel control. And if you have prolapsed organs, your doctor may recommend the insertion of a vaginal pessary, a plastic device that supports your organs.
In some cases, for instance, if you have an organ prolapse or significant incontinence issue, surgery may be the best option. Many procedures are outpatient surgeries. However, many experts recommend women avoid these surgeries until after they’re done with childbearing. Discuss your options with your health care team.
Conclusion
Whether you have symptoms or not, it’s worth learning more about the pelvic floor and its remarkable role in your body. If you’re experiencing uncomfortable symptoms, discuss how you feel and what to do about it with your health care provider. In some cases, earlier intervention may lead to swifter relief.